


|

|
|
TITHE AN OIREACHTAISSEVENTH JOINT COMMITTEE
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Table 2.1 VHI Health Insurance Plans and Premiums, |
|||||
|
|
|
August 1993* |
|
|
Plan |
Adult |
Child |
Family of Four |
Accommodation |
Hospital |
|
(£) |
(£) |
(£) |
|
Type |
A |
140 |
47 |
374 |
Semi-Private |
Public |
B |
195 |
71 |
532 |
Private Semi-Private |
Public Private** |
C |
300 |
116 |
832 |
Private |
Private** |
D |
358 |
141 |
998 |
Semi-Private |
MP/BC |
E |
537 |
217 |
1508 |
Private |
MP/BC |
Notes: |
|||||
MP=Mater Private; BC=Blackrock Clinic |
|||||
2.14A matter of considerable interest to the Joint Committee is whether the higher level Plans (i.e. D and E), which entitle subscribers to accommodation in the Mater Private and the Blackrock Clinic, are in any way subsidised by the lower level Plans. The VHI reports that the claims from subscribers to the D and E Plans exceed their subscriptions. However, the VHI in their response to this question point out that the major part of the difference in the higher cost of claims by D and E subscribers, as compared to A, B and C subscribers, is due to the higher average age of the former and only a small proportion is the result of the cost of accommodation in the Mater Private and the Blackrock Clinic. In this respect it should be noted that 70% of the claims from D and E subscribers are in respect of stays in public hospitals or private hospitals other than the Blackrock Clinic and the Mater Private. At the same time, B and C Plan subscribers are covered by the VHI for 90% of the cost of stays in the Mater Private and the Blackrock Clinic. In fact, the VHI states that when each of the Plans is evaluated on the basis of the age structure of the entire VHI membership, the procedure appropriate to community rating, the three higher schemes each yield a surplus over claims, and the two lower schemes yield deficits.
2.15Another innovation since 1979 was the introduction, in 1987, of schemes of insurance (Plans P and T) against the £10 per diem charge (subsequently increased to £20 per diem) introduced in the Budget of that year for stays in public hospitals. This charge is levied on that section of the public which, until then, had entitlements to free stays in hospitals (i.e. Categories II and III under the Health Acts which amounted to about 60% of the population). It should be noted that VHI subscribers to the Hospital Plans are automatically covered against these charges.
2.16In 1991 the Board partially addressed the problem of limited indemnity for doctors’ fees by the introduction of the “full cover scheme”. It negotiated a differential fee structure whereby doctors who accepted the VHI fee schedule as full payment for their services to subscribers (“participating doctors”), received a higher level of remuneration than those who did not. Subscribers attending these doctors therefore have 100% indemnity for both hospital charges and doctors’ fees. Doctors unwilling to accept the VHI schedule receive a lower payment and are free to charge their clients additional amounts. As of now 65% of all consultants are participating. (See Appendix III for a list supplied by the VHI of the consultants and specialists participating in the VHI’s total indemnity scheme)
2.17Finally, reference should be made to the abolition in 1991 under the Programme for Economic and Social Progress (PESP) of Category III status.1 The present position is that the entire population are entitled to free hospital and consultant care in the public wards of public hospitals. This actually abolishes one of the raisons d’être of the VHI: the provision of insurance for the cost of hospital care for persons with limited entitlements under the Public Health Acts. Since everyone now is entitled to free hospital care, the 15% of the population who were in Category III have less incentive to join the VHI. To restore the relative attractiveness of private health insurance, the VHI believes that it is important to be able to offer total indemnity to its members.
2.18The purpose of health insurance, and insurance generally, is to protect against “major and unforeseeable” costs. Excluded from the coverage of VHI schemes are:
•dental and ophthalmic treatment;
•services which are preventative in nature such as check-ups and health screenings;
•alternative and complementary treatments such as acupuncture, chiropracty or reflexology;
•“non-curative” treatment, including long term care and maintenance.
•cosmetic surgery and procedures relating to infertility or contraception;
•infectious diseases (which are treated free by the state in special hospitals).
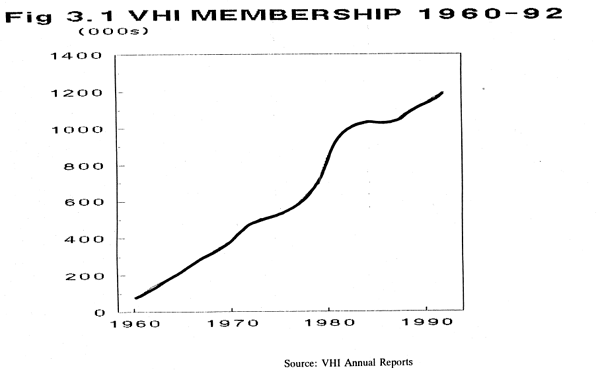
3.1The VHI commenced business in 1957 and membership rose steeply in the years immediately following (see Figure 3.1 below). The Advisory Body had estimated in its report that there were 450,000 persons with limited entitlements under the Health Acts who would be the “primary market” for the VHI. Within 5 years membership had reached 140,000 or the equivalent of nearly one third of the primary market - a remarkable penetration within such a short period of time. During the 1960s and 1970s, growth continued at a rapid rate nearly trebling by the end of the 1960s and doubling again in the 1970s at which point one person in four in the population was covered by VHI insurance.
3.2During the 1980s the rate of growth slowed down. Nevertheless, in the last thirteen years, the number of persons covered by the VHI’s main schemes of insurance has increased by 60% and the VHI now covers almost one in three persons. Considering the major changes which are now about to take place in the market for health insurance, and the need for appropriate responses by the VHI and the Department of Health, it is highly desirable to know as precisely as possible why people subscribe to the VHI in such large numbers. In the following paragraphs 3.3 to 3.8, available socio-economic data on VHI members are reviewed while the paragraphs after that consider data on why people join the VHI.
3.3Socio-economic statistics on the VHI’s members was published by the VHI on a regular basis in its annual reports up to 1984, at which point their publication ceased. The Joint Committee feels that this information helps public understanding of the role and performance of the VHI and recommends that it should resume the practice of publishing a range of relevant socio-economic indicators.
3.4Since 1984 the only supplementary information on members published by the VHI is their average age. Currently, this is 32.5, having increased from 30.1 seven years ago. The average age of VHI members is therefore rising at about one third of a year per annum. The implications of this for the future funding of the VHI are adverted to at paragraph 5.8.
Fig 3.1 VHI MEMBERSHIP 1960-92
3.5The only other socio-economic information on the VHI’s members which has been provided since 1984 was collected through a sample survey undertaken by the Economic and Social Research Institute (ESRI) in 1987 as part of a wide ranging study of health of health services utilisation in Ireland 2. This provides a more up to date and fairly comprehensive profile of the membership body.
3.6While it is true that the “typical” VHI member belongs to the professional and white collar social classes, enjoys a relatively high income, holds Category III status (or did so until the Category was abolished) and is in the active age group (say 35-54), the ESRI data reveal that there are significant exceptions to this.
1The majority of Category III members (74.1%) are members of the VHI, but a fairly high proportion (25.9%) are not, considering that this Category was liable for consultants’ fees. (see Table A.1 in Appendix II)
2A relatively high proportion (32.6%) of Category II who have entitlements to free hospital treatment are, nevertheless, members of the VHI. This group constitute the majority (59.8%) of the VHI’s membership. (see Table A.1 in Appendix II)
3There is a close association between income, when this is adjusted for family size, and membership of the VHI. Nevertheless, 25% of the top 10% of the population in income-adjusted terms are not members of the VHI. About 7% of the bottom 10% are VHI members. (see Table A.2 in Appendix II)
4As might be expected, there is a clear positive association between social class and VHI membership. But once again, there are significant numbers of the higher categories who do not have VHI cover (e.g. 30.8% of “Higher Professional/Managerial”) and significant proportions of the lower categories who do (e.g. 14.9% of “Skilled Manual”). (see Table A.3 in Appendix II)
3.7Examining VHI membership by reference to age reveals another important fact (see Table A.4 in Appendix II). While about 9.8% of the population are over the age of 64, only 6.3% of VHI subscribers are in that age category. In other words, there is an under-representation of the elderly by about one third. The under-representation of the elderly in VHI membership is contrary to the natural expectation that old people, with a high incidence of illness, would be more likely to take out health insurance than younger age groups. The same logic would suggest that the young would be under-represented but in fact the table shows that they are about proportionately represented among VHI subscribers.
3.8The obvious explanation for the lower participation of the elderly is that being on retirement incomes they cannot afford health insurance. However, there are other factors which help to explain the apparent lower participation of the elderly and the proportionate participation of the young:
1The elderly are survivors from a time when total participation in the VHI was low (i.e. the 1960s) and when far fewer people of all socio-economic categories participated.
2Simple membership of the VHI is probably not a fully accurate measure of participation. Allowance should be made for the type of membership. In fact, young people tend to opt for the lower insurance plans and older people for the higher ones.
3Some allowance also has to be made for the effect of the other licensed health insurance schemes, notably those of the ESB and the Gardai. These may have some share of older age groups or higher socio-economic categories which, if added to those in the VHI, might make participation in health insurance schemes in general more in line with the a priori expectations mentioned in paragraph 3.8.
3.9The ESRI study examined trends in VHI membership and in addition in 1990 conducted a special questionnaire survey in an additional effort to identify the reasons why people join the VHI. In the case of the membership data, the ESRI informally associated the increases over the years with changes in incomes and in the cost of subscriptions. During the 1960s and 1970s, rapid growth in membership of the VHI appears to be explicable in terms of rapid growth in disposable incomes. In the 1980s, the growth in disposable incomes slowed down but membership of the VHI continued rising, albeit at a diminished rate. Nevertheless, by the end of the decade, membership had increased by over one third. This is a very large increase considering that during the 1980s:
•Disposable incomes had risen by only 15% in real terms.
•The cost of subscriptions (as crudely measured by total subscriptions revenue divided by total membership) had risen by 250% in real terms.
•Entitlement to hospital services had been extended to Category III in 1979.
3.10In explaining the relatively rapid increase in membership in this period, the ESRI adduced the following explanations:
1Due to the large increase in the marginal rates of income tax during most of this period, the real cost of VHI subscriptions for many classes of subscribers probably changed very little.
2Restrictions in the availability of public health services, which the ESRI claimed were reflected in the decline in numbers of acute hospital beds and the fall in the real value of spending on hospitals, prompted individuals to take out health insurance.
3Eligibility for public health services is not a very strong explanation, in statistical terms, of membership of the VHI: the ESRI’s researches show that factors such as social class and income are more significant. Consequently the improvement in eligibility in 1979 would not have been likely to have had much effect. In any case, the VHI responded to the improvement in eligibility in 1979 with improvements in its own schemes. (See Paragraphs 2.10 to 2.12)
3.11The importance of 3.10 (2) above, i.e. access, is emphasised by a survey which the ESRI carried out in 1990 in order to complement its analysis based on the 1987 Survey. This was a sample survey of 1,000 households asking their principal reason for subscribing to the VHI. As Table 3.1 shows, the largest majority by far (62.4%) said that ready access to hospital care was the main reason. Other reasons, “being sure of getting good treatment” (9.6%), and being able to choose your own consultant (7.8%) were relatively insignificant.
Table 3.1 Reasons for Having VHI Cover |
|
||
Reasons for Having VHI Cover |
Percentage Stating: |
||
|
“most |
“next most |
“least |
|
important” |
important” |
important” |
Being able to have a private or semi-private room in hospital |
5.1 |
8.8 |
34.0 |
Being able to choose your own consultant |
8.3 |
17.2 |
6.6 |
Being sure of getting into hospital quickly when you need treatment |
62.4 |
13.9 |
1.1 |
Being sure of getting good treatment in hospital |
9.6 |
26.2 |
6.3 |
Being able to get into private hospitals |
2.1 |
4.4 |
26.7 |
Being sure of getting consultant care |
4.7 |
19.0 |
5.7 |
Being able to arrange hospital treatment for when it suits you |
7.8 |
10.5 |
15.5 |
Total |
100.0 |
100.0 |
95.9 |
Source:Brian Nolan, The Utilisation and Financing of Health Services in Ireland, Economic and Social Research Institute, General Research Series, Paper No 155, Dublin, 1991.
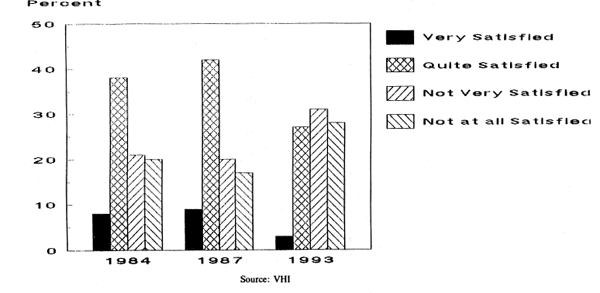
These findings are complemented by the VHI’s own market research, which in addition have detected a downward trend in public satisfaction with the public health services. (see Figure 3.2 below)
3.12The VHI, in its submission to the Joint Committee in 1991, stated its belief that with one in three persons in the country covered by its plans, it had achieved virtual “saturation” of the market. The ESRI’s data tends to suggest that as of the time of its survey, 1987, there was still some scope for expansion amongst the former Categories II and III. In fact, between 1987 and 1991 there was a further increase in the VHI’s “penetration rate” from 28% to 33%. Indeed, since the VHI’s submission in 1991, there have been further increases in the absolute and relative number of VHI subscribers. This suggests that, although rapid increases in the VHI’s membership in the future are unlikely, the “market” for private health insurance may be bigger than is commonly thought.
Fig 3.2 SATISFACTION WITH THE HEALTH SYSTEM
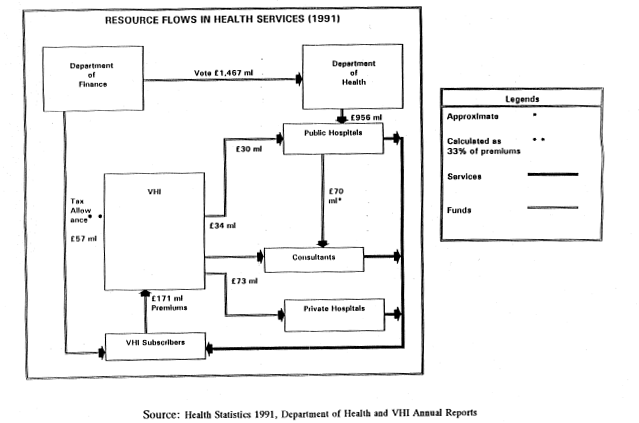
4.1Figure 4.1 below shows the role of the VHI, and private health care, in the financing and provision of health services in Ireland. The VHI is funded by subscriptions from VHI members. These are paid out to public hospitals for treatment of VHI members in pay beds and to consultants, most of whom work some or all of their time in public hospitals. The VHI also makes payments to private hospitals and to GPs and other specialists outside the hospital system. On the other hand members of the VHI benefit from the allowability against tax of their premiums. The value of this is probably something in the region of one third of the gross cost of the premium - a significant alleviation.
4.2In addition to the financial flows which are relatively easy to identify, there are also significant resource flows between the VHI members and the public sector which are not matched by financial transactions. The dimensions and the net direction of these resource flows are not easy to quantify. With respect to consultants, it seems to be generally accepted that without the possibility of earning fees privately, the public hospitals would not be able to attract the quality of consultants and in that case public patients would be at a loss. In that sense, the public sector is the beneficiary of the private.
4.3On the other hand, the Department calculates that the private patients are not being charged the “full economic costs” of the public hospital paybeds. There is therefore an implicit subsidy to the VHI subscribers. The Department regards the revenues from VHI members as an important contribution to the funding of the hospitals and is in the process of raising them to the “full economic cost” of the paybeds. (The issue of the amount of the paybed charges, together with details of the definition of “full economic cost” is discussed further in paragraphs 6.29 to 6.32) There is also a financial gain to the Department from the diversion from the public health services, of patients funded by the VHI attending private hospitals.
4.4The 1957 Act accords the following forms of control over the VHI to the Minister for Health:
•The Minister for Health appoints the Chairman and Directors of the VHI for five year periods but can remove them at any time.
•The approval of the minister is required for schemes of insurance.
•The Minister has the right to require the Board to provide schemes of insurance at his specific request.
4.5As mentioned in Paragraph 2.4 above, the level of reserves is a matter for the Board to decide and the 1957 Act permits the Board to determine the level of subscriptions so as to attain the targeted level of reserves. The two are therefore interrelated. In practice however, the Board defers to the Minister in determining increases in premiums. The Board has not always received the increases in the amounts it seeks or received them at the times requested.
4.6The VHI has no share capital and, in this respect, resembles a mutual insurance company where retained earnings surplus to reserve requirements are available for the benefit of members in terms of reduced premiums or improved benefits. This appears to be supported by the provisions of Section 4 of the 1957 Act. However, the imposition of the £3 million levy on the VHI by the Minister for Health in 1992 would suggest that the Department views the VHI’s reserves as the property of the Minister for Health and thus that they are not necessarily for the benefit of members.
4.7The full extent of the interrelationships between the public and the private sectors is not delineated by this brief account. But it is not surprising that the Department should exercise a high degree of control over the VHI. Indeed, the controls, both formal and informal are such as to place the VHI in a very different position vis à vis the Department of Health than most state companies in relation to their sponsoring Departments. In fact, a former secretary of the Department of Health referred to the VHI as “an arm of the Department of Health”.
4.8However, the Joint Committee feels that the exercise of these controls have to take account of two sets of concerns:
•the need of the VHI for a stable policy environment within which to develop the health insurance business;
•the need for the VHI to have an adequate degree of independence from the Department of Health.
4.9If the VHI is to conduct its affairs in an orderly and businesslike fashion, it must do so within a reasonably predictable environment of Government control and regulation. This means that there must be some fixed mechanism and criteria for allowing the VHI and other health insurers to increase premiums and for increasing paybed charges to health insurers. While the Government may have good reasons for requiring a greater contribution to the finances of the Department of Health, these contributions should be exacted within some medium-term framework. In its submission to the Joint Committee, the Department observed “…it is the Government’s policy to move gradually, with full regard to the VHI’s financial position, to a level of VHI reimbursement to public hospitals which reflects more accurately the real costs of delivering care and treatment to semi-private and private patients.” (emphasis added). The subsequent imposition of the levy and later increases in paybed charges, all of which have to be recovered from members through increases in premiums, do not seem to have taken adequate account of the VHI’s finances nor of its need for a stable financial environment.
4.10Apart from the financial difficulties, the Department’s decision making on the levy and paybed charges complicates the VHI’s task of negotiating with doctors and private hospitals. It is obviously difficult for the VHI to convince these groups that there is no room for improving its rates of payment when it is obliged, without warning, to fund large payments to the Department.
4.11Another example of how unanticipated demands of this sort can complicate the management of the VHI was brought to the attention of the Joint Committee by one of the representatives of the Independent Hospital Association of Ireland (IHAI). The Government’s levy, which was given statutory effect by the 1992 Finance Act, came at a time when the VHI was defending a case in the High Court brought by one of the private hospitals. It was a material point in the VHI’s case that it was a non profit organisation. Yet the payment of £3 million to the VHI’s effective owner seemed to some IHAI members to support the case that the VHI had profits to dispose of.
4.12The VHI in its submission to the Joint Committee has expressed the view that it is, in effect, if not in form, a mutual organisation for the benefit of its members. That is probably also the view of the members themselves. However, the Department, which has the objective of increasing revenue from the VHI for public hospitals, exerts considerable control over the VHI. Should it wish to do so, it is in a position, through its influence over the VHI’s insurance schemes, premiums and reserves, to ensure that the VHI gives a higher priority to the financial needs of the public hospitals.
4.13Public hospitals are, in effect, in competition with private hospitals for VHI patients. This competition is a powerful one, since the public hospitals already cater for about half of the VHI’s members. The public hospitals have attracted considerable investment in recent years and the best are a match for the best of the private hospitals in terms of facilities and personnel. The Department is in a position, through its influence over the VHI, to place the private hospital sector at a disadvantage. In fact, the representatives of the private hospitals feel that the regime imposed on them by the VHI is preventing investment in the sector which, if continued, would leave them unable to provide private patients with the service that they demand. The VHI’s relations with the private hospitals are discussed in Chapter 6. But at this point it is enough to say that it is desirable that the VHI should be seen to be independent as between the use of private and public hospitals.
4.14Finally, in the emerging competitive environment it will eventually be impossible for the Department to treat the VHI any differently to any other health insurer. Market competition, if it is effective, will narrow the options open to the Department in respect of the VHI’s schemes of insurance, levels and use of reserves and rates of premiums, matters in which the Department has intervened in the past. The means to strengthen the VHI’s independence are discussed further in Chapter 8.
4.15The Joint Committee feels that it would be helpful if the forthcoming legislation, which is planned to implement the Third Non Life Directive, assigned responsibility for the supervision of health insurers, including the VHI, to the Department of Enterprise and Employment which already has responsibility for overseeing all other insurance companies subject to the Insurance Acts. The question of reserves would then be a matter for that Department.
4.16The Department of Health, on the other hand, would retain responsibility for the development of the health insurance industry including premiums and schemes. But power which now exists in the 1957 Act to direct the VHI to adopt particular schemes of insurance should be replaced by powers over health insurers in general. Furthermore, these powers should be exercised within an explicit, medium term planning framework for the industry, including details about the timing, magnitude and bases for charges for public sector paybeds and criteria for permitting increases in subscriptions (if this power is retained under the new legislation).
4.17The provision of the Finance Acts which allow subscriptions to licensed health insurers to be allowable against tax is an important financial contribution from the public sector to VHI members and, of course, to the members of other health insurers. The nominal value of the concession is estimated by the Revenue Commissioners from time to time and at the moment is probably not less than one third of the value of subscriptions or about £60 million in the case of the VHI. Whether this exceeds the benefit of the VHI to the public sector is difficult to prove statistically. In the absence of the tax concession, VHI membership would drop to some degree, as would revenues to the public hospitals, while at the same time costs to the public sector would increase as former VHI subscribers switched from private hospitals and invoked their public health entitlements.
4.18However, although no formal evaluation has been made of its net economic effect on the public sector, the tax concession on VHI subscriptions has attracted criticism from a number of prestigious bodies including:
• the Commission on Taxation (1982);
• the National Planning Board (1984);
• the National Economic and Social Council (1986);
• the Commission on the Funding of the Health Services (1987);
• the Department of Health (1987);
• the Industrial Policy Review Group (the Culliton Committee (1992)).
4.19Despite the recommendations of these bodies, successive Governments have not altered the concession and statements in such documents as, for instance, the Programme for Economic and Social Progress, 1991, indicate that it is unlikely that any change will take place in the near future. However, the concession is given for subscriptions to health insurers holding a licence. As things stand this means the VHI and a small number of other insurers. After next year it will be possible for other companies to apply for and receive licenses. These may be private sector Irish companies or foreign enterprises. In that context the concession may not seem so acceptable. At the minimum there may be further pressure to reduce the value of the concession to, say, the standard rate of tax rather than the marginal, or to restrict it to one of the lower plans.
4.20The view of the Joint Committee is that the tax allowance for health insurance premiums is cost effective in encouraging private individuals to take out insurance and so generate revenue through paybed charges and divert demand from the public hospital services. It is true that VHI membership has shown considerable resilience in the face of increases in subscriptions in the past. But the withdrawal of the tax allowance would result in after tax increases ranging from about one third (in the case of the standard tax payer) to about 100% (in the case of the marginal tax payer). These increases would be in addition to increases due to ongoing inflation and the impact of increased charges for paybeds. In the circumstances the Joint Committee believes the withdrawal of the tax concession would be likely to have a significant adverse effect on membership and therefore recommends its retention. The cautionary remarks by Nolan are worth bearing in mind in this context.3
5.1In the period since the Joint Oireachtas Committee last examined the VHI, claims have risen from £20 million to £190 million, an increase of 850% or 18.1% per annum. Deflated by the Consumer Price Index, this is an increase of 270%. By way of comparison, current public expenditure rose by 13% in real terms and total personal incomes by 27%. The factors behind this inflation include those which underlie the phenomenon of medical inflation throughout the world, together with some matters specific to the VHI:
•an increase in membership of 45%;
•the introduction of the new insurance “products” in the shape of the Mater Private Hospital and the Blackrock Clinic from 1986 onwards;
•other new technologies and procedures;
•ageing of the VHI membership: the VHI calculates that an increase of one year in the average age of membership increases claims by 4.2%; VHI average age rose by 2.7 years between 1986 and 1993;
•general inflation in wages, salaries and consumable materials in the health sector;
•consultants’ fees;
•increases in public hospital paybed charges and, in the early 1980s, withdrawal of the Department of Health subsidy to private hospital beds.
5.2Table 5.1 below shows that VHI premiums rose from £25 million to £196 million between 1980 and 1993.4 This was an increase of 632% in money terms. Deflated by the Consumer Price Index this works out at an increase of 270%. Like the growth in claims, this is an extraordinarily rapid rate of increase. The ability of the VHI to push up its premiums by such high rates testifies to a strong position in the market even when allowance is made for the availability of tax relief on its premiums.
Table 5.1. Financial Performance of the VHI 1980-93: Profitability |
||||||
Year |
Subscriptions |
Claims |
Administration |
Underwriting |
Surplus |
Return on |
|
|
|
Expenses |
Profit/Loss |
Deficit |
Net Assets |
|
(’000s) |
(£m) |
(£m) |
(£m) |
(£m) |
(%) |
1980 |
25.2 |
19.6 |
2.3 |
3.3 |
5.5 |
51.9 |
1981 |
30.3 |
27.5 |
3.3 |
-0.5 |
3.7 |
26.4 |
1982 |
39.2 |
38.6 |
3.8 |
-3.2 |
0.5 |
2.0 |
1983 |
57.3 |
59.5 |
5.2 |
-7.4 |
-0.3 |
10.8 |
1984 |
74.9 |
76.0 |
5.3 |
-6.4 |
1.3 |
1.2 |
1985 |
88.5 |
86.9 |
5.7 |
-4.1 |
2.4 |
10.7 |
1986 |
99.8 |
97.3 |
6.3 |
-3.8 |
6.9 |
25.1 |
1987 |
112.0 |
110.4 |
7.0 |
-5.4 |
2.9 |
9.9 |
1988 |
126.4 |
141.6 |
8.5 |
-23.7 |
-12.3 |
-70.3 |
1989 |
145.0 |
155.4 |
9.5 |
-19.9 |
-11.3 |
-171.2 |
1990 |
158.7 |
147.7 |
11.4 |
-0.4 |
6.2 |
48.4 |
1991 |
171.2 |
160.0 |
13.0 |
-1.8 |
8.8 |
41.3 |
1992 |
183.1 |
172.9 |
14.0 |
-3.8 |
8.4 |
28.4 |
1993 |
195.9 |
190.4 |
12.6 |
-7.1 |
5.8 |
15.7 |
Source: VHI, Annual Reports.
5.3As in the case of most insurance companies, the VHI usually experiences an underwriting loss: that is the cost of claims and administrative expenses exceeds subscription income. In the period under review, such losses were incurred in all but one year. This represents a deterioration by comparison with most of the VHI’s history since, in the period up to 1980, underwriting losses were incurred about every other year. The overall surplus or deficit represents the difference between the underwriting loss (profit) and income from investments, including gains realised from the sale of investments. Since 1980 there were only three years in which such losses were incurred but two of those years, 1987 and 1988, witnessed significant losses. Prior to 1980, the VHI recorded deficits in only four years and in none were the losses significant.
5.4The only available measure of return on capital is the surplus as a percentage of net assets and this shows a high degree of volatility arising from the fluctuations in profit. Over the fourteen years 1980-93 the VHI earned an aggregate surplus of £28.5 million which represents an average rate of return of 10.5% on net assets.
5.5The liquidity of a company is the extent to which it is in a position to meet its immediate liabilities. It is usually measured by the ratio of current assets to current liabilities. Obviously, if current assets are less than current liabilities, i.e. the current ratio is less than 1.00, the VHI could be in danger of being unable to meet claims bills should there be any sudden deterioration in trading conditions. In fact, even in 1989, Table 5.2 below shows that the VHI did not reach that situation.
Table 5.2 Financial performance of the VHI 1980-93: Liquidity and Solvency |
||||||
Year |
Current |
Current |
Current |
Net Assets |
Target |
Reserves as Ratio |
|
Assets |
Liabilities |
Ratio |
(= Reserves) |
Reserves |
of Target Reserves |
|
(£m) |
(£m) |
(Ratio) |
(£m) |
(£m) |
|
1980 |
31.0 |
21.1 |
1.47 |
10.6 |
4.1 |
2.58 |
1981 |
37.9 |
24.2 |
1.57 |
14.4 |
5.8 |
2.49 |
1982 |
47.6 |
33.8 |
1.41 |
14.8 |
8.1 |
1.83 |
1983 |
64.0 |
50.7 |
1.26 |
16.6 |
12.5 |
1.33 |
1984 |
75.8 |
62.1 |
1.22 |
16.8 |
16.0 |
1.05 |
1985 |
89.2 |
73.8 |
1.21 |
18.7 |
18.2 |
1.02 |
1986 |
105.0 |
80.8 |
1.30 |
27.5 |
20.4 |
1.35 |
1987 |
118.2 |
92.2 |
1.28 |
29.3 |
22.8 |
1.29 |
1988 |
130.4 |
117.1 |
1.11 |
17.5 |
26.9 |
0.65 |
1989 |
132.3 |
130.2 |
1.02 |
6.6 |
31.4 |
0.21 |
1990 |
108.5 |
93.9 |
1.16 |
12.8 |
34.2 |
0.37 |
1991 |
136.7 |
110.9 |
1.23 |
21.3 |
35.8 |
0.59 |
1992 |
158.1 |
132.3 |
1.20 |
29.6 |
37.0 |
0.80 |
1993 |
164.1 |
131.6 |
1.25 |
36.9 |
40.3 |
0.92 |
1991: Change in accounting policies affects statement of current assets and current liabilities Target Reserves: 1987 to 1993 are as stated by VHI Board. 1980 to 1986 are 2.5 month’s claims. |
||||||
Moreover, the VHI is possibly less exposed to such hazards than general insurance companies since the incidence and cost of claims is fairly predictable in the short term. In addition, the VHI’s strong market position and the tax allowability of its subscriptions make it easier for the VHI to recoup any losses through increasing its subscriptions (assuming Government approval is granted). Finally, the fact is that the VHI is a state enterprise and usually has no borrowings so that temporary finance would be readily available were it ever needed to fund short term cash outflows.
5.6The largest part of the VHI’s current liabilities are pending claims and unexpired subscriptions. On the other hand, the largest part of its current assets are cash and short term deposits which are readily realisable. The company also maintains a portfolio of Government securities which are highly liquid. Investments in equities, property and other assets which might be less freely realised are usually a small proportion of the total portfolio amounting, in 1993, to 2% of the total. The current ratio of the VHI started the 1980s at around the 1.50 mark but declined to nearly 1.00 after the losses of 1988 and 1989. It has since recovered to about 1.25. Before 1988, the VHI’s current ratio stood at 1.28 and the swift decline to virtually 1.00 in the two succeeding years suggests that the 1993 current ratio of 1.25 is not unduly generous.
5.7A measure of solvency for a general insurance company is the ratio of claims to reserves. Minimum solvency margin requirements are laid down by the European Communities (Non-Life Insurance) Regulations, 1976. The VHI is exempted from such requirements at the moment. Nevertheless, the Board, which is required to maintain such reserves as it deems reasonable, aimed at the ratios required of all general insurance companies. Since 1987 the Board has published the minimum reserves required but in only one year has the Board reached the target and that was in 1987. Since the low point in 1989, when they reached £6.6 million, the VHI has made considerable progress in reconstituting its reserves. Nonetheless, at the end of 1993, it was still short £3.4 million. From July 1994 onwards, the VHI will not be exempt from the Insurance Companies Acts and will be obliged to maintain the minimum reserves specified.
5.8It is appropriate at this point to advert to the impact on the VHI’s finances of the ageing of its membership and to raise the issue of the desirability of a special reserve against the increase in the cost of claims attributable to this factor in the future. As noted in paragraph 3.4, the average age of the VHI’s membership is 32.5 and is rising at the rate of one third of a year per annum and this rate of ageing adds about 1.4% to the VHI’s claims. The VHI is funded on a “pay-as-you-go” basis so an age reserve is not appropriate. The constitution of such a reserve might be justified even for a “pay-as-you-go” scheme, if a very steep increase in claims due to ageing was anticipated. However, the VHI’s membership is fairly representative of the general population and ageing will be gradual. That is a situation which could change if the advent of competition were to lead to the defection from the VHI of a substantial number of younger subscribers. But the Joint Committee does not consider that a likely contingency, especially if the recommendations which follow are adopted.
5.9There are two aspects to the efficiency of the VHI. The first, and most important, is the extent to which the VHI ensures that its subscribers get a cost effective service from the providers of health care: doctors and hospitals. The second aspect of the VHI’s efficiency is the extent to which, given the claims from subscribers, the VHI is cost effective in the use of its own resources. The second aspect is dealt with in the following paragraphs while the first aspect is dealt with in Chapter 6.
5.10There are two measures of efficiency derivable from the VHI’s annual reports. These are shown in Table 5.3:
Table 5.3 Measures of Efficiency of the VHI: 1981-92 |
||
Year |
Administration/Claims (%) |
Average Number of Claims per Staff Member |
1981 |
12.00 |
521 |
1982 |
9.84 |
611 |
1983 |
8.74 |
651 |
1984 |
6.97 |
688 |
1985 |
6.56 |
713 |
1986 |
6.47 |
714 |
1987 |
6.34 |
740 |
1988 |
6.00 |
716 |
1989 |
6.11 |
754 |
1990 |
7.72 |
769 |
1991 |
8.13 |
717 |
1992 |
8.10 |
729 |
1993 |
6.62 |
764 |
Administration expenses as a percentage of claims is a frequently quoted indicator of efficiency in insurance companies. The VHI’s rate was around 12% at the beginning of the decade, but fell fairly steadily until 1988 when it reached 6%. The ratio subsequently increased to 8.1% in 1992, but declined again in 1993. By the standards of general insurance companies the VHI’s administration expense ratio of 6.6% in 1993 is extremely low. It may be noted that the increase in the ratio from 1988 to 1992 was due to increased expenditure on information systems. These are investment-type outlays in that they are not recurring and should yield benefits in later years.
5.11Factors which help the VHI to maintain a low expense ratio include the simple nature of its insurance product range; its simple risk assessment procedures (open enrolment and community rating); limited expenditure on advertising due to the absence of competition; and the contribution to administration made by voluntary administrators of group schemes. A factor which, on the other hand, contributes to the VHI’s cost structure to a degree not likely to be found in general insurance companies, is the need to maintain close surveillance of hospital costs and consultants’ fees. The large investment in information technology referred to above has enabled the VHI perform these functions with maximum cost effectiveness.
5.12The average number of claims handled by each employee is another measure of efficiency. The final column in Table 5.3 above shows that this ratio increased from 521 claims per employee in 1981 to 764 in 1993 - an increase in productivity of 46.6%, which compares well with other service activities.
5.13The losses which took place in the VHI’s profits in 1988-1989 were attributed by the VHI to the following factors:
• the establishment of two new “high tech” hospitals (the Blackrock Clinic and the Mater Private Hospital);
• the rapid increase in out patient drug costs;
• general private hospital costs;
• consultants’ fees;
• price control of premiums;
• increased charges for public hospital paybeds.
5.14According to the VHI several of the factors leading to the deficits in 1988-1989 were outside its control. The VHI resisted the establishment of the two “high tech” private hospitals but evidently succumbed to pressure to include them in its schemes. The cost of the drug scheme also remained uncontrolled for a period of time and of course the charges for public pay beds is a matter for the Department of Health. This is also the case for increases in the subscriptions which were either disallowed or delayed by the Department.
5.15A start was made on the reconstitution of the VHI’s reserves through a programme of measures including:
• the discontinuance of the out patient drugs scheme;
• an increase in subscriptions;
• a standstill or in some cases a reduction in public and private hospital prices;
• a reduction in fees to certain specialist consultants;
• day care was made mandatory for certain conditions.
5.16 As illustrated in Table 5.1 above, the result was a drop in the underwriting loss, the re-emergence of a surplus and a rapid recovery in the level of reserves, though not, as of the end of 1993, to the level desired by the Board. In addition in the last two years, the Government has taken steps which have had some adverse affect on the VHI’s financial situation including the imposition of a levy of £3 million payable from the VHI’s reserves and increases in the paybed charges in public hospitals. However, due to investment income, the Board has recorded a surplus of £5.8 million in the year ended February 1993. This still leaves reserves below the desired level, but the VHI expects that it should attain the required level of reserves by the end of the current year (i.e. the twelve months ending February 1994).
5.17 It is a matter of some concern, however, that since the stabilisation of the VHI’s finances in 1990, the underwriting losses have increased in each of the succeeding three years. This reinforces the ongoing need for the VHI, consultants and hospitals, private and public, to exercise strict cost control.
5.18It seems relevant to add one final point about the losses which the VHI incurred in 1988 and 1989. The VHI reports that according to its regular opinion surveys, public opinion about the VHI deteriorated sharply during this period. This is an outcome of the curtailment of services, increases in premiums and also the bad image which losses convey. To the usual financial reasons there are, therefore, to be added cogent marketing reasons for the VHI to avoid losses.
6.1There are 1,100 doctors holding consultant positions in public hospitals. Under their contracts with the Health Boards they are paid a salary which, at the present moment, is around £65,000 for a 33 hour week. To this can be added a number of supplementary payments. On the other hand many consultants work considerably in excess of their required 33 hours.5 These consultants are entitled to have a private practice outside this time. Some of their clients will be treated in pay beds. But sometimes these consultants will hold posts in private hospitals where they will treat their private patients. In addition to these consultants there are also about 150 doctors who are wholly engaged in the private sector holding consultant positions. VHI benefits also extend to non-consultant practitioners including GPs for certain services provided outside the hospital environment. Altogether, the VHI pays fees to about 2,500 practitioners. (See Table 6.1)
Table 6.1 VHI Disbursements 1984-93 |
|||
Year |
Public Hospitals (including levies) |
Private Hospitals |
Doctors Fees |
|
(£’000s) |
(£’000s) |
(£’000s) |
1984 |
14,978 |
30,788 |
18,658 |
1985 |
17,511 |
33,917 |
20,799 |
1986 |
21,656 |
37,747 |
23,876 |
1987 |
22,425 |
46,017 |
25,367 |
1988 |
25,464 |
62,058 |
28,550 |
1989 |
30,013 |
65,970 |
31,317 |
1990 |
29,879 |
66,428 |
31,989 |
1991 |
30,102 |
72,898 |
33,959 |
1992 |
33,844 |
82,353 |
36,398 |
1993 |
640,722 |
91,493 |
41,280 |
6.2Initially, the VHI simply paid a scale of fees to consultants which was believed to be in line with the “going rate” for each procedure. However, the consultants tended to keep their fees about 15% to 20% above the VHI rates. The result of this was that patients found that they were in effect underinsured. The “balance bills” which results from this are strongly resented by its members according to the VHI, and generate unfavourable perceptions of the VHI. An extent of balance billing is given in Table 6.2 below.
Table 6.2 Comparison of Consultants’ Charges and VHI Payments 1984-93 |
|||||
|
|
|
(£ Million) |
|
|
Year |
Charges |
VHI Payments |
Balance Bill |
Index of VHI |
Index of |
|
|
to Consultants |
as % VHI |
Payments to |
Consumer |
|
|
|
Payment |
Consultants* |
Prices |
1984 |
22,080 |
18,658 |
18.3 |
100.0 |
100.0 |
1985 |
24,233 |
20,799 |
16.5 |
110.9 |
106.7 |
1986 |
28,162 |
23,876 |
18.0 |
127.4 |
111.9 |
1987 |
30,660 |
25,367 |
20.9 |
134.7 |
115.5 |
1988 |
34,837 |
28,550 |
22.0 |
145.9 |
119.1 |
1989 |
37,742 |
31,317 |
20.5 |
155.8 |
122.3 |
1990 |
38,544 |
31,989 |
20.5 |
156.0 |
128.1 |
1991 |
42,639 |
33,959 |
25.6 |
160.6 |
131.5 |
1992 |
46,067 |
36,398 |
26.6 |
168.1 |
136.2 |
1993 |
50,851 |
41,280 |
23.2 |
190.6 |
139.4 |
1994** |
60,402 |
49,718 |
21.5 |
|
|
6.3In 1991, as part of an effort to eliminate balance billing, the VHI introduced a reformed fee schedule based on an assessment of the amount of time required to carry out a given procedure with some allowance for training, experience and costs. Under this schedule higher rates were paid for consultants who agreed not to balance bill their patients. After intense negotiations, 57% of the consultants agreed to participate in this scheme.
6.4 For patients attending these consultants, there is, therefore, total indemnity. The 1991 agreement was for a period of two years and was renegotiated in early 1993 and as of the time of writing 65% of the consultants were participating 6. Table 6.3 following gives details on the current state of the VHI’s negotiations with the different groups of consultants. (See Appendix III for a list supplied by the VHI of consultants and specialists participating in the VHI’s total indemnity scheme).
Table 6.3 Participating and Non-Participating Consultants |
||||
Speciality |
Number of |
Percentage |
Number of |
Percentage |
|
Consultants |
Participating |
Consultants |
Participating |
|
1991-93 |
1991-93* |
1993** |
1993** |
Physicians |
486 |
77 |
485 |
88 |
Surgeons |
514 |
36 |
529 |
53 |
Radiologists |
99 |
96 |
101 |
96 |
Anaesthetists |
218 |
31 |
218 |
31 |
Pathologists** |
46 |
98 |
46 |
0 |
6.5The consultants’ representatives submitted to the Joint Committee that their relations with the VHI were poor. From their viewpoint the difficulty was an unwillingness on the part of the VHI to negotiate realistic rates for fees. In particular they felt that:
The VHI makes no allowance for practice expenses.
There are a number of anomalies in the schedule.
A high proportion of consultants’ claims are “pended”, meaning queried for one reason or another by the VHI.
The VHI’s surveillance of claims threatens the patient/doctor relationship.
6.6The Joint Committee has no means available for determining whether the demands of the consultants are reasonable or whether, on the contrary, the VHI is making unrealistic offers. In the first place, it is not easy to determine what the earnings of consultants are. Table 6.4 below gives a schedule of fees paid to consultants by the VHI in the year ending February 1993. It can be seen that the highest consultant was paid £220,000 by the VHI and that about half the total was paid to just 200 consultants. In assessing these figures it should be remembered that the majority of the consultants are also in receipt of a salary of about £65,000 by virtue of their appointments to public hospitals. The receipts from balance bills, and from private patients not insured by the VHI, also have to be taken into account. On the other hand allowance has to be made for practice expenses such as professional insurance, secretarial services, accommodation and office supplies.
Table 6.4 Stratification of Consultants’ and Doctors’ Earnings from the VHI, 1993 |
|||
Range |
Number of |
Average Earnings (£) |
Percent Share of |
(£000s) |
Consultants/Doctors |
|
Total |
83 - 274 |
100 |
112,882 |
27.3 |
61 - 83 |
100 |
71,307 |
17.3 |
46 - 61 |
100 |
53,395 |
12.9 |
38 - 46 |
100 |
41,611 |
10.1 |
31 - 38 |
100 |
34,331 |
8.3 |
24 - 31 |
100 |
27,300 |
6.6 |
17 - 24 |
100 |
20,531 |
5.0 |
13 - 17 |
100 |
15,422 |
3.7 |
9 - 13 |
100 |
11,498 |
2.8 |
6 - 9 |
100 |
7,628 |
1.8 |
0 - 6 |
1,550 |
1,090 |
4.1 |
|
2,550 |
41,280,460 |
100.0 |
6.7 The VHI has pursued the objective of total indemnity for a number of reasons:
1Demand:
VHI members complain vigorously about the practice of being billed for a service after, as they see it, having paid for it in advance through their VHI subscriptions. In seeking to eliminate balance billing the VHI is therefore responding to demand.
2Competition:
Free treatment in public hospitals is available to everyone, and the VHI needs to maintain the relative attractiveness of its services. Balance billing is a serious flaw in the VHI’s “product”. This may become a more significant disability in the context of an open market next year.
3 Cost Control:
Without some means of limiting the upward movement of consultants’ fees (i.e. a “ceiling”) there is a risk that the VHI’s reimbursement rates will simply be a “floor” which will enable consultants to charge a higher overall fee. In the extreme case a consultant could add a balance bill equivalent to the fee which he would have charged in the absence of VHI reimbursement. In that case, the VHI subscriber is not insured at all.
6.8 The Joint Committee endorses the VHI’s policy of attempting to get total indemnity from consultants. However, the Joint Committee is concerned at the cost of the policy. It must be remembered that in order to get consultants to accept total indemnity the VHI has to offer a higher rate to all participating consultants, including those who had been accepting the existing VHI schedule. Moreover, as Table 6.2 shows, the incidence of balance billing was actually smaller before 1991, when the VHI commenced negotiations with the consultants on total indemnity, than it was in 1993, when 65% of consultants were participating.
6.9 Table 6.5 below shows that within the overall total of balance billing the incidence has changed over the years as between the different specialities. The bulk of it used to be accounted for by surgeons but in recent years it has tended to become a more general phenomenon with anaesthetists taking a more assertive posture. The differing incidence of balance billing amongst the specialities reflects the perceptions and aspirations of the groups concerned.
Table 6.5 Incidence of Balance Billing between Specialities |
|||||||||
|
|
(Balance Bill as % of VHI Payment) |
|
|
|
||||
Speciality |
1984 |
1986 |
1988 |
1990 |
1991 |
1992 |
1993 |
1994 |
1994 |
|
% |
% |
% |
% |
% |
% |
% |
%* |
£ml* |
Surgery |
26.9 |
25.9 |
28.7 |
17.8 |
18.7 |
25.8 |
23.6 |
19.1 |
26.6 |
Anaesthesia |
14.5 |
16.2 |
35.2 |
60.6 |
70.3 |
67.8 |
54.9 |
56.9 |
6.3 |
Physicians |
11.6 |
10.4 |
14.2 |
17.4 |
21.1 |
20.4 |
16.6 |
11.9 |
8.6 |
Radiology |
1.2 |
0.9 |
1.0 |
10.8 |
17.0 |
12.4 |
5.7 |
5.2 |
4.4 |
Pathology |
3.3 |
3.4 |
3.6 |
16.5 |
56.3 |
10.6 |
3.3 |
20.5 |
3.8 |
Total |
18.0 |
17.8 |
22.0 |
20.5 |
25.6 |
26.6 |
23.2 |
21.5 |
49.7 |
6.10 However, the 1991 agreement with the consultants expired in 1993 and was replaced with a new one under which the VHI succeeded in raising the percentage of participating consultants to 65%. It is perhaps encouraging to note that in the first half of this year (i.e. the period March to August), the incidence of balance billing has declined from the level in the preceding year (i.e. down from 23.2% to 21.5%). However, in percentage terms it is still about as high as it was prior to 1991 and the absolute amount, around £10 million, has remained unchanged since 1991. This suggests that the effort to control the consultants’ fees will need to be supplemented by other initiatives. These are considered next.
6.11To prevent the “elevator” effect of VHI reimbursement rates the VHI has suggested that Government regulation of consultants’ fees should be considered. Needless to say the consultants’ organisation strongly rejected any such suggestion pointing out that regulation does not apply to other professions in Ireland. Regulation of doctors and consultants fees does exist in a number of countries including, for example, the Netherlands, Australia and France. In the latter two countries certainly, it does not appear to be very successful. The Joint Committee does not consider state regulation of fees to be a very practical suggestion.
6.12Two other means of putting countervailing pressure on consultants’ fees include:
(1)The exclusion of non-participating consultants from the scope of VHI plans is likely to be counter productive in the context of a relatively small market with limited alternative possibilities for consultants (or the VHI) to find alternative insurers (consultants).
(2) The publication of the names of participating consultants amongst VHI members has been resisted by the profession in the past, but the Joint Committee can see little valid objection. The names of participating hospitals are circulated to VHI members. The Joint Committee therefore recommends that the VHI circulate the names of participating consultants to its members by whatever means seem effective. (See Appendix III for a list supplied by the VHI of consultants and specialists participating in the VHI’s total indemnity scheme).
6.13 Moreover, it might be helpful to define a role for a third party in negotiations between the consultants and the VHI. At the present moment discussions between the two sides seem to proceed with considerable acrimony, no doubt related to the fact that the consultants have only one insurer to negotiate with. In addition, from the public point of view it is undesirable that such negotiations should be completely obscured from public scrutiny.
6.14 It is suggested therefore that an independent assessor/ombudsman should be appointed who would take into account all the necessary information, including information about consultants’ costs and incomes of comparable professions, and who would also make recommendations made about fee scales (Similar recommendations are made to deal with hospital charges and proposals for new hospitals and equipment in paragraphs 6.27 and 6.38 and it is desirable that the same assessor should deal with all three types of issue). The recommendations could be non-binding (unless the parties agree otherwise) but the grounds on which the recommendations were made would be publicised and the independence and expertise used in the procedure would give the recommendations considerable moral authority. The incomes of many groups in Ireland are governed by procedures which are a good deal more restrictive than this.
6.15There are 32 private hospitals in Ireland, the majority of which are owned by religious orders and are run for charitable purposes. There are also three hospitals which are owned by consultants and private investors. Their objectives are to provide opportunities for professional practice or for earning profits. The range of facilities offered by private hospitals varies enormously and includes establishments providing recuperation facilities, day surgery up to and including the two high tech hospitals in Dublin providing the most sophisticated facilities. The Independent Hospitals Association of Ireland (IHAI), which represents 20 of these hospitals, estimates that the private hospitals have 2,200 beds and treat about 250,000 patients each year involving a total of 750,000 bed days of care. About 90% of the cases handled by the private hospitals are VHI subscribers and account for about half of all hospital care purchased by VHI subscribers.
6.16 In the past the VHI used to negotiate day rates with each of the hospitals which varied from hospital to hospital depending on the range and quality of the facilities offered. In 1991, following the implementation of the recovery plan the VHI introduced an alternative regime. Under this each hospital was assigned a quota of cases as well as a daily rate thus effectively capping each hospital’s earnings. Subsequently, this was modified in that cases over and above the quota would be permissable but would be reimbursed on a marginal cost basis which was from 25% to 40% of the average. (In succeeding years the extra cases could be taken as part of the hospital’s “base load”). The daily rate payable took account of each hospital’s “case mix” so that hospitals handling complex cases would not be penalised. The rates provided for a profit margin of 3% on turnover with additional payments for approved capital expenditures.
6.17Other features of the VHI regime which drew objection from the IHAI were
• the VHI’s insistence that hospital management accounts be submitted regularly to the VHI;
• the VHI is in a position to delist the hospitals altogether if they do not accept VHI conditions;
• a condition of their agreements with the VHI that the private hospitals, unlike non-participating consultants, are not allowed to balance bill their patients 7;
• the stated desire of the VHI to have the powers to engage in the running of hospitals creates a conflict of interest for the VHI and gives rise to the suspicion that the VHI may be attempting to force some hospitals out of existence in order to facilitate the entry of the VHI into hospital activities.
6.18 According to the IHAI:
• The quotas do not reflect the demand from VHI subscribers. Consequently VHI subscribers are being denied treatment. The IHAI estimates that the number so denied amounts to 4,000 cases.
• The cash limits resulting from the regime do not take account “of the nature and cost of care provided” - an assertion which seems to conflict with the VHI’s claim that their reimbursement system takes account of case mix.
• The rates of reimbursement are below the “economic levels” and have contributed to the fact that, according to the IHAI, the independent sector has incurred losses of £10 million in the 1989-91 period.
• Private hospitals are unable to generate sufficient profits to enable them to invest in new facilities. The IHAI asserts that there is “…clear evidence of demand and need in key regional centres” and that “private funding of £30 million would be available to construct new hospitals providing 300 beds or 100,000 bed days”.
In conclusion the IHAI states that the VHI’s “…cost containment policies have exceeded their intended effect and now operate to the disadvantage of VHI’s own subscribers and may in effect be designed to reduce the private hospitals to a position of financial peril…”.
6.19 The IHAI recommends:
• the elimination of the financial restrictions imposed by the VHI;
• the recognition by the VHI of the need of the hospitals to earn an adequate return so as to provide for replacement and upgrading of equipment and buildings;
• the recognition by the VHI and the Department of Health that the private hospital sector has a role to play in the national health context;
• the VHI to negotiate with the hospitals “…in a spirit of constructive cooperation… to achieve their mutual objectives of providing quality patient care…”
6.20 In assessing the case made by the IHAI the Joint Committee is in a parallel situation to that which it is in in respect of the consultants: there is a deficiency of information. However, the Joint Committee does not accept all of the points submitted by the IHAI. In particular, the un-met demand for 100,000 bed nights quoted by the IHAI does not seem to square with the IHAI’s figure of 4,000 cases turned away each year, which is also denied by the VHI. However, while there may be doubt about the exact numbers, the Joint Committee is convinced, from members’ contacts with constituents, that there is a shortage of capacity to treat private patients.
6.21 This particularly appears to be the case in the mid-west where there is no private hospital in an area comprising 327,000 persons. In addition, the public hospitals in the region lack the capacity to treat private patients. Consequently, VHI subscribers in this area seeking treatment must travel to Galway, Kilkenny or Cork. The Joint Committee is aware that proposals have been submitted to the VHI from private groups for the establishment of private facilities in the region but these have been rejected by the VHI. The Joint Committee regards this rejection as an arbitrary use of its powers by the VHI and considers that to the extent that VHI subscribers are obliged to travel long distances for treatment, they are not receiving the service from the VHI for which they paid.
6.22 The Joint Committee also notes that the absence of capacity in the public hospitals in the region is contributing to the absence of services for private patients, as well as public patients, and urges that the Department of Health take the necessary steps to remedy the situation.
6.23 As far as the financial situation of the private hospitals is concerned, ideally, the Joint Committee would like to have seen information on the aggregate financial accounts of the private hospitals including details on capital spending over recent years. However, the Committee is inclined to believe that the financial situation facing private hospitals as a whole is difficult. Hospitals, unlike consultants, do not have contracts with the public sector for any part of their revenues. In addition, hospitals have physical assets to maintain and improve and, in a period of financial stringency provisions for replacements and renewals are likely to be the first items to suffer. The private hospital sector could also be at a disadvantage vis á vis its larger public sector competitor.
6.24 The Joint Committee also accepts that the regime which the VHI has developed for controlling private hospitals is not satisfactory in the long run. In effect, the VHI is virtually administering the private hospitals in influencing the volume of business they do, their levels and types of staffing and the amount and types of capital spending they undertake. This gives reduced scope for commercial freedom including freedom and the incentive to compete for business and to pioneer new services. A consequence of this may be a slowing down in the rate of technical progress and growing rigidity in cost structures. It also contributes to the situation where the mid-west region remains with no private hospital facilities.
6.25 Of course in using these controls, the VHI is in the same situation as that of many private health insurers in other countries who are under the same pressures to limit the increase in claims. Accordingly, the Joint Committee feels that the suggestion from the IHAI that the VHI should virtually abandon its controls over the volume and cost of hospital treatment is unrealistic.
6.26 However, there are countervailing pressures on the side of the hospitals. If the VHI is to retain its members it will have to have the services of private hospitals. It is therefore in the VHI’s interests to ensure that there is a viable, well equipped private hospital sector. In Chapter 4 the Joint Committee has outlined recommendations for helping to ensure that the VHI, and any other health insurers that there may be in the future will have the necessary policy framework within which to encourage the private sector.
6.27 The Joint Committee also feels that it would be useful that claims for costs by the hospitals, and other matters of dispute between the hospitals and the VHI, could be submitted to the independent assessment procedure proposed for the consultants. (See paragraph 6.14). It is possible that the assessor/ombudsman might have to have access to different types of expertise when considering matters relating to hospitals as opposed to matters relating to consultants.
6.28 At the moment about half of the VHI’s members are treated in private hospitals and half in public hospitals. Under the 1991 PESP it was agreed that beds for private patients would be formally designated and distinguished from public beds. As of the present moment there are 2,360 of these which is approximately the same as in the independent sector. However, the capacity of the public sector to handle private patients is actually somewhat larger because there are also a number of beds which are available for private and public patients and private patients can also be accommodated in public beds pending the availability of private beds. This latter is a situation which would arise in respect of emergency admissions.
6.29 The Department charges VHI subscribers a daily rate for private patients in public hospital paybeds. The rate is inclusive of all costs of hospital care (i.e. accommodation and ancillaries) apart from consultants. This rate varies depending on the type of hospital with the highest rates being charged for pay beds in the teaching hospitals. According to the Department these rates are below the “full economic cost” of the beds and the Department proposes to increase its charges to the VHI gradually to the point where the economic rate is recovered.
6.30 The full economic cost of a public hospital bed in this context refers to the total annual cost of that hospital divided by the total number of bed days. Excluded from total costs in this calculation are those costs not relevant to private patients such as salaries of consultants and non consultant doctors and the costs of out-patient and emergency services. Another item which is excluded from this definition are the capital costs of the hospital (interest, depreciation, debt repayments) since these are not charged to the Department of Health but are absorbed by the Exchequer.
6.31 The VHI reports that even at the moment, the rates paid to many private hospitals are below the full economic cost for public hospitals, and also that they include some provision for the capital costs of private hospitals which, as noted in the preceding paragraph, the Department does not have to take into account in calculating the rates for public hospitals. If the rates for public hospitals are increased to the full economic cost, the net effect will be to make the private sector more price competitive with the public sector. There will then be little difference between the cost of the VHI’s Plans A and B (for semi private and private accommodation in public hospitals) and the higher plans (for accommodation in private hospitals). Since the standard of semi private accommodation in public hospitals is often indistinguishable from public accommodation, there will tend, over time, to be a switch among VHI members to the private plans and a drop in the public hospitals’ “business”.
6.32 The difference between the existing cost to the VHI for paybeds and the costs at full economic rates is £18 million. If implemented in full the VHI’s costs would rise by that amount if, against expectations, public paybed business continues unchanged. If there was a switch to the use of private hospitals, then the increase in the VHI’s costs would be somewhat less, though still very significant, given that many private hospitals are charging less than the Department’s full economic cost.
6.33 In addition, it has been argued by the VHI and the consultants that it is unfair to private patients to charge them the full economic cost of private accommodation rather than the marginal costs given that everyone is entitled to care in a public ward. In effect, by opting for private care, the private patient forfeits all entitlements under the Public Health Acts. In those public hospitals where there is, in fact, little difference between the accommodation of public and private patients, this practice seems less justifiable. But in any case the Department’s policy in this area differs to that followed in the other areas of Government policy where, like health, there are major redistributive objectives: education and social welfare. Parents who send their children to private post primary schools still get the benefit of the Department of Education’s subsidy for teachers’ salaries (though the benefit of other subsidies available to “free” schools and public post primary schools are not available). In the case of social welfare, people do not lose their entitlements to unemployment benefits and contributory pensions by “topping” them up with redundancy payments, the earnings of spouses, the proceeds of life insurance policies, occupational pensions or other savings.
6.34 Marginal costs of paybeds calculated on this basis are likely to be extremely low-considerably lower than the rates charged even now by the Department of Health. But charges fixed on this basis would render the private hospitals highly uncompetitive. To be fair to them, the Department of Health would have to subsidise beds in the private sector to the amount equivalent to the value of public health entitlements. This would introduce a “voucher” concept of entitlements which would be a major change in social distribution principles in Ireland and in practice would involve a substantial addition to the expenditures of the Department of Health.
6.35 The question of the charges to be made for paybeds cannot be seen in isolation from the general relationship which should exist between public and private hospitals. At the present moment about half of the VHI’s subscribers are treated in public hospitals and about half in private hospitals. The Joint Committee believes that the current balance as between the two is reasonable and should as far as practicable be maintained. Indeed, there may be scope for the private hospitals to provide services for public patients when, as happens from time to time, capacity in the public sector is inadequate. The services of the MRI scanners (referred to in paragraph 6.37 below) made available by the private sector to the public sector is an example of this cooperation. The recent contracting out of orthopaedic work by the Southern Health Board is another example of the scope which may exist, even though in this particular instance the work went to Northern Ireland rather than to private hospitals in the Republic.
6.36 The Joint Committee’s recommendation is that the Department of Health has to fix the charges it makes to the VHI at a rate which does not cause VHI patients to shift from public hospitals to private hospitals and so maintains the existing balance. The other constraint which has to be respected is the possibility that the impact of paybed charges (along with other costs) on the level of the VHI’s premiums will cause people to drop out of the VHI altogether. Both of these considerations suggest to the Joint Committee that paybed charges are now at approximately their correct relationship to private hospital charges.
6.37 The VHI has adopted a number of approaches to the control of costs:
The VHI has invested heavily in recent years in computerised systems. These allow the VHI to handle a larger volume of claims with the same number of, or fewer, employees. It also allows the VHI to monitor claims for reimbursements by individual hospitals and by practitioners.
The VHI endeavours to control expenditure with incentives for cost effective practices. This includes incentives to divert patients to day surgery, to reduce the average length of stay in hospital and to transfer post operative patients from expensive acute hospitals to lower cost convalescent hospitals.
The VHI also keeps downward pressure on costs through limiting the “proliferation” of facilities in the form of extra bed capacity or extra equipment. Tight control on capacity ensures that there is little scope for supplier induced demand. Of course, if the VHI applies too much pressure the result will be that genuine needs will go un-met. This is, in fact, the case urged by the IHAI. And there have been occasions when the VHI has been obliged to provide coverage for facilities which it felt were excessive most notably in the case of the two high tech private hospitals. The VHI felt that one high tech hospital would have been sufficient. In its submission, the VHI has pointed out that there is no official hospital licensing system in Ireland which would help ensure that supply of facilities was in line with demand.8
6.38 The danger with an official licensing system for hospitals is that it could rigidify the hospital system and suppress the introduction of technology. As in the case of the Joint Committee’s recommendations about reimbursement of hospitals and consultants, a solution might be to submit to independent assessment procedures all proposals for new technologies and facilities, including the required number of beds in the private and public sectors. Since there are similarities in the assessment of reimbursement claims from hospitals and consultants and the assessment of the cost effectiveness of medical facilities, the assessor/ombudsman should be the same for all three. However, as noted in paragraph 6.27, the expert advice available to the assessor/ombudsman might vary somewhat depending on the issue before him or her.
6.39 In its Corporate Plan, the VHI has outlined additional methods for improving cost effectiveness of the services provided for its members by consultants and hospitals. Three initiatives which the VHI is preparing seem to the Joint Committee to be particularly noteworthy:
The VHI proposes to encourage private hospitals to introduce arrangements for reviewing the outcome of treatments so as to identify and promote best practice among consultants;
The VHI proposes to strengthen its computerised systems for monitoring the cost of different treatments from hospital to hospital and practitioner to practitioner. Variations in costs will be readily identifiable and communicated to providers to encourage adoption of cost effective treatments.
The VHI proposes to help hospitals to develop information systems which will improve hospital decision making and facilitate communication of claims between the hospitals and the VHI.
6.40 The VHI’s proposals to implement improvements in its own systems and those of the hospitals in order to enhance cost control and to promote peer review in order to promote best practice, are strongly endorsed by the Joint Committee. The Joint Committee looks forward to reviewing the benefits of these initiatives on the next occasion that it examines the VHI.
7.1 Although it was not recommended in the Advisory Committee report, nor is it incorporated in the 1957 Act, it has generally been accepted that the VHI, to be effective, would have to be a monopoly. The 1957 Act requires that applicants must hold a licence from the Department of Health to provide health insurance and it has been the practice since the VHI was established to refuse applications for such licences.
7.2 With entry to the European Community, and the programme to create a single market, there has been increasing harmonisation of member states’ insurance industry regulations as well as measures for opening up member states’ insurance markets to insurers from other member states.
This established common rules for calculating solvency margins and made it easier for insurers from one member state to establish in another. However, member states were permitted to exempt certain institutions from these regulations and the Irish Government exempted the VHI.
Insurance companies were permitted to offer insurance in other member states without having an establishment in other member states. In these cases, responsibility for ensuring that solvency margins are respected rests with the “home” country. The VHI was exempted from the provisions of this Directive also.
This abolishes the exemptions so that from July 1994 the VHI and health insurance in general will be exposed to the rigours of the First and Second Directives. However, largely at the insistence of the Irish Government, the Directive provides that member state Governments can require health insurers to market policies based on the principles of community rating, open enrolment (anyone can join) and life time membership (membership cannot be withdrawn on age grounds). These insurers do not have to be established in Ireland.
7.3 Three aspects of competition among health insurers are worth considering in some detail:
• the control of risks and the pricing of subscriptions;
• the range of insurance products on offer to the market;
• the cost effectiveness of insurers contracts with health providers (i.e.doctors and hospitals).
7.4 The VHI’s subscriptions are based on the community rating principle. That is, everyone pays the same health insurance premium irrespective of their risk of making a claim. These risks rise progressively with age so that community rating involves a transfer from the young to the old. This transfer is justified on social grounds because the old are judged to be more vulnerable economically than the young. In the VHI’s Plans there are some limits to the principle: people over 65 cannot join the VHI while all have to go through a waiting period before gaining eligibility for benefit. Conditions existing prior to membership are not claimable. But subject to that, the VHI premiums are the same; anyone can join and can remain a member for life.
7.5 The opposite to community rating is risk rating, whereby premiums are calculated in relation to the probability that a class of subscriber will make a claim. In a competitive environment it is believed that new entrants to health insurance, whether domestic or foreign, would offer lower risk related schemes which would mean lower rates for young people. Young subscribers would thus be attracted away from the VHI which would eventually be left with the higher risks (“cherry picking”). The VHI would, therefore, have to raise its rates to very high levels to remain solvent. This would constitute an unfair burden on older subscribers.
7.6 It could be argued that the VHI has such a strong “hold” on the market that new entrants would make little impression on the VHI’s finances and so enable community rating regime to continue, even in a market open to entry by competitors. This may well be the case in the initial stages of the open market. But the evidence from the UK and Australia is that a community rating insurer will eventually be vulnerable to competition from a risk rated competitor. If community rating is to be preserved, some regulatory mechanism will be required.
7.7 Before going on to consider the form of regulation, it is as well to consider arguments against community rating which have been put forward by the consultants and/or the private hospitals:
1Community rating encourages adverse risk selection. The bad risks are encouraged to join by the relatively (i.e. relative to their risk of claiming) low cost while the good risks are deterred by the relatively high cost. This means that overall costs are likely to be higher than under a risk related scheme. However, given that one third of the population are members of the VHI it seems to the Joint Committee that any extra cost must be relatively small. Indeed, the evidence from the ESRI report8 is that VHI members have a higher, not lower, health status than the rest of the population.
2 Having been deterred from joining the VHI in their youth by high premiums, some people never join, thus depressing the potential number of insured persons. However, as noted in paragraph 3.7, the young are proportionately represented in the membership of the VHI which does not give much support for this argument - even when allowance is made for the point in paragraph 3.8 (2) that the young are under represented in the VHI’s higher Plans.
Table 7.1 Age Related Premia |
|
(on basis of community rating=100) |
|
Age |
Age Specific Rate |
20 |
33 |
30 |
90 |
40 |
90 |
50 |
100 |
60 |
125 |
70 |
225 |
80 |
275 |
90 |
325 |
This is based on the VHI’s |
A Plan and includes males and females. |
7.8 The Joint Committee’s view is that community rating is a principle worth defending. Certainly, a fully risk-rated system, which would rate subscribers according to very fine age groups would not be acceptable. As Table 7.1 indicates, under a risk rated system, an 80 year old would have to pay nearly three times the average (i.e. community) rate. Also, the elderly have been net contributors to the VHI during their younger days and so have a moral, if not a legal, entitlement to be net beneficiaries in their old age. Finally, the VHI’s membership now embraces a very large proportion of the population, many of whom, as Chapter 3 indicates, are from the middle income groups. This justifies the use of restrictions which protect subscribers from the full impact of a freely competitive market.
7.9 The regulation of the Irish health market to ensure that, in a competitive environment, community rating can be preserved gives rise to a number of technical problems. It might be thought that cherry picking could be avoided by simply requiring all insurers to offer open enrolment and lifetime membership. This would mean that insurers would be obliged to take and keep subscribers as they apply and, therefore, they will not be able to refuse the higher risks. However, insurers can market their products at particular segments of the market and, while not refusing what they consider to be bad risks, can ensure that the majority of subscribers are in the desired category. For example, insurers could attract younger people by directing their marketing effort at employers whose workforces tend to be below the average age.
7.10 In countries which have sought to combine competition and community rating, it has therefore been necessary to introduce an equalising financing mechanism or compensation fund (in Australia this is termed the reinsurance fund). In principle, the mechanism is simple: insurers report their claims expenses for those over a certain age (in Australia this is 65) and those insurers which have less than the average number of 65 plus year-olds in their membership pay a levy into the compensation fund, while those who have more than the average 65 plus draw out a subsidy. There is, therefore, no incentive for the competing funds to use the techniques referred to in the preceding paragraph to evade elderly subscribers (open enrolment and lifetime membership are obligatory in Australia).
7.11 In practice, however, the Australian compensation fund has not totally eliminated the scope for cherry picking and even more sophisticated systems based on a range of factors additional to age and chronic illness could be open to manipulation by insurers.9 While in the early years of the open market it is not likely that any distortion in the equalisation mechanism would make a great deal of difference to the VHI, in the long run a fairly sophisticated mechanism will have to be implemented.
7.12 However, one major drawback inherent in the compensation fund concept is that it is difficult to apply it to more than one health insurance scheme. For example, it would not be practical to devise a scheme for each of the VHI’s five insurance Plans, still less for the multiplicity of plans which may emerge in a competitive market. The consequence of this is that it will be necessary to define a “basic” plan which all insurers must offer and which will be eligible for funding from, or obliged to make payments to, the compensation fund. The VHI’s B Plan, which provides for semi-private accommodation in ordinary private hospitals and private accommodation in public hospitals, has the largest number of subscribers and is likely to be the basic insurance scheme.
7.13This could mean that all insurance schemes other than the basic one would be excluded from the operations of the compensation fund and would thus, under the force of competition, eventually become fully risk rated. However, an alternative arrangement would be that all health insurance schemes would be subject to the compensation mechanism to the extent that their costs do not exceed those covered by the basic scheme. This would mean that only that fraction of the costs of, for example, the D Plan, which is attributable to accommodation in the Mater Private or Blackrock Clinic, would be risk rated, while the bulk of the subscriptions would remain community rated. The Joint Committee is of the opinion that the compensation mechanism, and, by implication, community rating, should be applied to all health insurance schemes (excepting the “ancillaries” mentioned below) to the extent that the costs of these schemes do not exceed the costs of the basic scheme.
7.14 If the community rating principle is safeguarded, that means that one form in which competition will take place will be product diversity. In addition to basic polices covering hospital and consultants’ fees, companies will compete by offering supplementary insurance for GPs’ visits, drugs, dental treatment, unorthodox therapies (acupuncture, reflexology, etc). These would widen consumer choice and so be a welcome addition to the Irish market. In the interests of preserving the drain on the Exchequer, and not giving undue artificial encouragement to the growth in health care expenditure, it might not be desirable that health insurance premiums for these ancillaries be eligible for tax relief. The Joint Committee would certainly visualise that the VHI would extend its range of insurance products to cover some of these ancillary forms of insurance, if it is necessary to meet the competition.
7.15 One other way in which competition can manifest itself under a community rating regime is through insurers negotiating lower charges for their subscribers with health providers: hospitals and consultants. Given that consultants, the Department of Health and the private hospitals are anxious to increase their charges, there would not seem to be much scope for this form of competition in the Irish case. It might, however, be a factor in the long run and if so, it would be a welcome countervailing force to the on-going pressures of medical inflation.
7.16 However, given the known objection by the public to balance billing it is more likely that competition will include offering total indemnity for consultants’ fees. Though expensive, such policies could be popular and affordable by relatively high income groups. Unfortunately, policies of this kind might reinforce inflationary tendencies which the Joint Committee believes are already latent in the area of professional fees. The Joint Committee understands that the Government has not yet decided whether it will continue to exercise control over the level of premiums. However, the Joint Committee believes that it would be desirable for the Government to retain powers to enable it to intervene to control the level of premiums, should it appear that medical inflation was getting out of hand.
8.1 The advent of competition, whether in an actual or potential form, will dramatically change the environment in which the VHI will be operating. From a monopolistic enterprise, it will have to become a fully competitive market oriented organisation. This will call for considerable cultural and organisational change within the VHI. It will also call for changes in the State’s controls over the VHI. However, the VHI was established as a statutory corporation under the close jurisdiction of the Department of Health with the responsibility for administering schemes of health insurance and not much else. This is no longer an adequate framework for the future. It is understood that the Department of Health, in conjunction with preparing legislation for the protection of community rating, is also considering a major revision to the 1957 Act. This chapter makes recommendations about changes to the 1957 Act and about changes within the VHI.
8.2 In its submission to the Joint Committee the VHI asked that it should have the powers to engage in:
• all forms of health-related insurance such as cash schemes (“permanent health”) and holiday health insurance;
• ownership and/or operation of health care facilities including in-patient and out-patient and facilities for the elderly;
• the provision of insurance for care for the elderly;
• the development of work site “wellness programmes” and health screening;
• the sale of information technology services based on expertise built up internally by the VHI;
• the development of overseas business generally.
8.3 In terms of the 1957 Act, these activities would require changes permitting the VHI to raise finance, make loans, create subsidiaries, engage in activities other than health insurance schemes as prescribed in Section 4 of the 1957 Act, and undertake activities overseas.
8.4The Joint Committee endorses the wish of the VHI to expand the scope of its activities and suggests that the simplest method of proceeding would be to change the VHI from a statutory corporation to a company incorporated under the Companies Acts or a cooperative formed under the Friendly Societies legislation (the issue of ownership and control is discussed below). The memorandum and articles of association would then specify the activities which could be carried on by the VHI and which could include all of the foregoing. The contents of the memorandum and articles could be changed simply by resolution, should there be any requirement to do so in the future.
8.5 The IHAI and the consultants have expressed strong objection to the VHI becoming involved in the operation and ownership of hospitals. Their objection is on the grounds that the VHI would have a conflict of interest as between obtaining the best terms for its own members from the existing private hospitals and ensuring the viability of its own hospitals. It would also be in a position, through the use of its existing powers, to squeeze the profitability of the private hospitals and inhibit their development, thus making them vulnerable to competition from the VHI’s hospitals. Indeed, the IHAI seemed to indicate that the VHI might already be engaged in such a policy.
8.6 The VHI have stated that they would only wish to enter the hospital sector if the closure of some existing institution were to leave its subscribers without access in some part of the country. In this context, the VHI referred to the decline in religious vocations which, the VHI felt, might eventually lead to the closure of some of the private hospitals. But the VHI also adverted in its submission to the role of the for profit private hospitals which, it claimed, have a tendency to raise costs. There may be some implication here that the VHI might seek to inhibit the development of this segment of the hospital sector, if necessary by directly intervening itself.
8.7The Joint Committee’s view is that the VHI has or will have enough powers to encourage the provision of hospitals by private groups and that unless there evolved some compelling competitive reason, the VHI should not become directly involved in the provision of hospital services because:
• the conflict of interest argument put forward by the private hospitals seems to the Joint Committee to be a valid argument;
• hospital ownership and operation are not areas of VHI expertise.
8.8The corollary of this recommendation is that the VHI may have to accept that future development of health services probably will be through private for profit groups. Indeed, given the cost of funding modern medical facilities, and the consequent need for profitability, it is likely that there will eventually be not much difference in the modus operandi of charitable and for profit hospitals.
8.9 On the other hand the Joint Committee endorses the VHI’s intentions of becoming involved in health promotion schemes, ancillary insurance schemes and the sales of information technology. As the example of the ESB’s sale of treasury management and project management expertise has shown, internally generated skills of state companies can be successfully marketed at home and abroad.
8.10 At the present moment, the VHI has no share capital but is in effect owned by the Department of Health. As has been pointed out elsewhere in this report, the VHI is in an invidious position vis á vis private hospitals and consultants by virtue of its ownership and control by the Department of Health. But ownership and control of the VHI could place the Department itself in a difficult situation when a competitive market emerges. In these circumstances the Joint Committee believes there is a case for a change in the VHI’s status. The options would appear to be the following:
•Formation as a company under the Companies Acts and privatisation
The advantage is that the new enterprise will have full commercial flexibility, access to capital, a clearly defined management structure and clearly defined objectives. The main disadvantage is that the VHI is, and will remain for a considerable period, the largest factor in health insurance. In the Joint Committee’s view, it is not acceptable, either to members or health service providers, for it to be subject to a profit motivation.
• Formation as a cooperative
This could incorporate commercial flexibility and would correspond closely to the existing structure and ethos of the Board. The disadvantage is that with a widely dispersed membership, the election of appropriate directors and the appointment of managers could prove to be a problem - as appears to have been the case for several building societies. On balance, the Joint Committee would not favour the formation of the VHI along cooperative lines.
• Conversion from its present status as a statutory corporation into a state owned company incorporated under the Companies Acts.
This gives the VHI the flexibility of a commercial legal framework but retains the public interest ethos which would be lost in a privatised entity. The dangers from too close identification of the VHI with the Department of Health, mentioned in Chapter 4 could be minimised by the arms length arrangements discussed in paragraphs 4.15 and 4.16 and also by new criteria for appointing Directors. (See paragraph 8.11 below). On balance, the Joint Committee favours the change of the VHI into a state company.
8.11The 1957 Act specifies that the VHI Board should consist of five directors. This does not seem to the Joint Committee to be sufficient and it recommends that this be expanded to nine. It is desirable that there should be an explicit requirement that a majority of the VHI’s Directors should be mainly representative of members’ interests. This would help ensure the VHI’s independence of Government. Indeed, and pending expansion of the Board of the VHI, and any change in its legal status, the Joint Committee recommends that at least two and not more than three of the Directors of the VHI should be appointed as representatives of members’ interests.
8.12 The VHI was constituted and for the last 36 years has operated as a monopoly supplier of health insurance with a limited range of functions. From next year it will face the threat of competition. However, if the Joint Committee’s recommendations on scope of activities are accepted, the VHI will also have a much wider range of options. This will call for major change in the organisation, staffing and “culture” of the organisation. In particular, the VHI will have to become a market oriented company. The Joint Committee recommends that the VHI should undertake the necessary recruitment and training to position itself to respond to these challenges and opportunities.
8.13 The Joint Committee appointed Mr. Jim Dorgan of Curtin Dorgan Associates as its consultant for the purpose of this inquiry. The Joint Committee wishes to express its deep appreciation of the invaluable assistance given by him in the preparation of this report.
The Joint Committee would also like to thank Mr. Tom Ryan, Chief Executive of the VHI, for his very extensive assistance in the preparation of this report including the supply of documentary and statistical material, attendance at meetings of the Joint Committee and a number of interviews with the Joint Committee’s consultant.
The Joint Committee would also further wish to acknowledge the assistance of Mr. Jerry O’Dwyer, Assistant Secretary, Mr. Dermot Smith, Principal Officer, and Mr. Patrick Byrne, Assistant Principal of the Department of Health. Mr. Kevin Heery, General Secretary of the Independent Hospitals Association of Ireland and Chief Executive of the Galvia Hospital and Mr. Walsh, Chief Executive of the Bon Secours Hospital in Cork, also helped by attending a session of the Joint Committee and by giving a number of interviews to the Joint Committee’s consultant. The Joint Committee would also like to thank Mr. Finbar Fitzpatrick, General Secretary of the Irish Hospital Consultants Association for providing evidence to the Joint Committee and assisting the Joint Committee’s consultant. The Joint Committee is also indebted to the other representatives of the Independent Hospitals Association of Ireland, the Irish Hospital Consultants Association, the Irish Medical Organisation and the MSF trade union for attending sessions of the Joint Committee.
(Signed) LIAM KAVANAGH, T.D.
Chairman of the Joint Committee.
19 January, 1994
The VHI’s financial year ends at the end of February of each year. In this report references to VHI data for a particular year should be understood to refer to the twelve months ending at the end of February of that year. |
* Based on group rates; individual rates are approximately 10% higher.
** Excluding Mater Private and Blackrock Clinic.
1 Stationery Office, Programme for Economic and Social Progress, 1991.
2 Brian Nolan, The Utilisation and Financing of Health Services in Ireland, Economic and Social Research Institute, General Research Series, Paper No 155, Dublin, 1991.
3 Brian Nolan, The Utilisation and Financing of Health Services in Ireland, Economic and Social Research Institute, General Research Series, Paper No 155, Dublin, 1991
4 The VHI’s financial year ends at the end of February (see note on page 1).
5 A.D.Tussing, Irish Medical Care Resources: An Economic Analysis, Economic and Social Research Institute, General Research Series, Paper No 126, Dublin, 1985.
* Index of VHI payments to consultants in money terms divided by the number of VHI members to give an approximate indication of the trend in the unit cost of treatment. This index take no account of quality changes in treatments provided by consultants.
** Actual for first half of the year multiplied by 2.
6 December 1993
* At end of period.
** Numbers refer to practices.
* 1994 % based on half year March to August 1993, £ml based on fees paid to consultants in half year multiplied by 2.
7 The VHI maintains that the hospitals have the option of being non-participating and so retaining the right to balance bill in the same way as consultants. In practice the private hospitals opt for participating status.
8 The existence of three MRI scanners in the private sector for 1.3 million private health subscribers might be an example of proliferation since it has been suggested that 1 MRI scanner per million persons should be sufficient. The heavy demand experienced for these machines does not mean that there is not over capacity: some of the demand is from public patients pending the installation of a scanner in Beaumont Hospital and in other cases the availability of capacity has generated use which would not normally be justified.
8 Brian Nolan, The Utilisation and Financing of Health Services in Ireland, Economic and Social Research Institute, General Research Series, Paper No 155, Dublin, 1991.
9 van de Ven, W.P.M. and van Vliet, R.C.J.A., How Can We Prevent Cream Skimming in a Competitive Health Insurance Market,Second World Congress on Health Economics, Zurich, September 1990.


